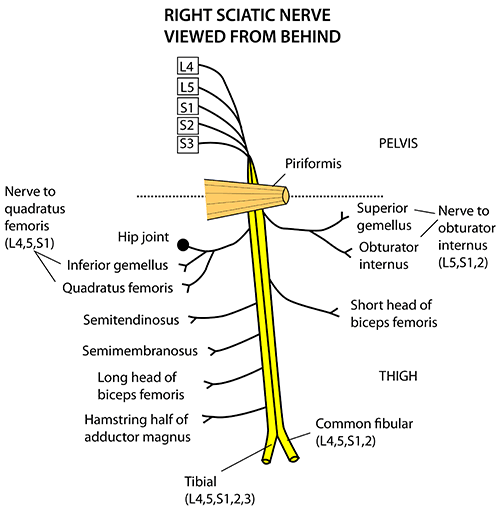
Sciatic nerve
The sciatic nerve is derived from the lumbosacral plexus. After its formation, it leaves the pelvis and enters the gluteal region via greater sciatic foramen. It emerges inferiorly to the piriformis muscle and descends in an inferolateral direction. As the nerve moves through the gluteal region, it crosses the posterior surface of the superior gemellus, obturator internus, inferior gemellus and quadratus femoris muscles. It then enters the posterior thigh by passing deep to the long head of the biceps femoris.
Within the posterior thigh, the nerve gives rise to branches to the hamstring muscles and adductor magnus. When the sciatic nerve reaches the apex of the popliteal fossa, it terminates by bifurcating into the tibial and common fibular nerves.
Anatomical variation: the sciatic nerve can be described as two individual nerves bundled together in the same connective tissue sheath – the tibial and common fibular nerves. These usually separate at the apex of the popliteal fossa, however in approximately 12% of people they separate as they leave the pelvis.
Click image to enlarge
Motor function
Although the sciatic nerve passes through the gluteal region, it does not innervate any muscles there. However, the sciatic nerve does directly innervate the muscles in the posterior compartment of the thigh (biceps femoris, semitendinosus and semimembranosus), and the hamstring portion of the adductor magnus.
The sciatic nerve also indirectly innervates several other muscles, via its two terminal branches:
- Tibial nerve – the muscles of the posterior leg (calf muscles), and some of the intrinsic muscles of the foot.
- Common fibular nerve – the muscles of the anterior leg, lateral leg, and the remaining intrinsic foot muscles.
In total, the sciatic nerve innervates the muscles of the posterior thigh, entire leg and entire foot.
Sensory function
The sciatic nerve does not have any direct cutaneous functions. It does provide indirect sensory innervation via its terminal branches:
Tibial nerve – Innervates the posterolateral and anterolateral sides of the leg, and the plantar surface of the foot (the sole).
Common fibular nerve – Innervates the lateral leg and the dorsal surface of the foot.
Clinical relevance
Pain caused by a compression or irritation of the sciatic nerve by a problem in the lower back is called sciatica. Common causes of sciatica include the following lower back and hip conditions: spinal disc herniation, degenerative disc disease, lumbar spinal stenosis, spondylolisthesis, and piriformis syndrome.
Other acute causes of sciatica include coughing, muscular hypertension, and sneezing.
Injury
Sciatic nerve injury occurs between 0.5% and 2.0% of the time during total hip arthroplasty. Sciatic nerve palsy is a complication of total hip arthroplasty with an
incidence of 0.2% to 2.8% of the time, or with an incidence of 1.7% to 7.6% following revision. Following the procedure, in rare cases, a screw, broken piece of trochanteric wire, fragment of
methyl methacrylate bone cement, or Burch-Schneider metal cage can impinge on the nerve; this can cause sciatic nerve palsy which may resolve after the fragment is removed and the nerve freed.
The nerve can be surrounded in oxidized regenerated cellulose to prevent further scarring. Sciatic nerve palsy can also result from severe spinal stenosis following the procedure.
Sciatic nerve injury may also occur from improperly performed injections into the buttock, and may result in sensory loss.
Other disease
Bernese periacetabular osteotomy resulted in major nerve deficits in the sciatic or femoral nerves in 2.1% of 1760 patients, of whom approximately half experienced complete recovery within a mean of 5.5 months.
Sciatic nerve exploration can be done by endoscopy in a minimally invasive procedure to assess lesions of the nerve. Endoscopic treatment for sciatic nerve entrapment has been investigated in deep gluteal syndrome.
isolated neuritis of the sciatic nerve in a case of Lyme disease https://www.ncbi.nlm.nih.gov/pubmed/10935841