GHB
Name:
GHB, 'G', liquid E, Gamma Hydroxy Butyrate
Effects:
Intoxication, increased energy, euphoria, increased talkativeness, desire to socialize, mild disinhibition, enhanced sexual experience, muscle relaxation.
Side effects:
Nausea, vertigo, headaches, drowsiness, confusion, loss of muscle tone, loss of coordination.
Mechanism of action:
GHB is a precursor to GABA, glutamate, and glycine. Acts as agonist on the GHB receptor (excitatory) and as a weak agonist at the GABA(B) receptor (inhibitory). It is a naturally occurring substance that activates oxytocinergic neurons in the supraoptic nucleus. Low doses stimulate dopamine release through GHB receptor, but higher doses inhibit dopamine release through GABA(B). Clinically, individuals may experience a paradoxal rebound effect, suddenly waking from a GHB induced sleep when GHB is eliminated and serum levels drop.
GHB is absorbed orally, with peak concentrations and effect occurring within 1 to 2 hours. The onset of action is rapid and may be as early as 15 minutes after ingestion.
GHB is rapidly metabolised via the Krebs cycle to water and carbon dioxide (see figure). A small amount is excreted unchanged in the urine where it may be detected for up to 4 to 6 hours. The elimination half-life of GHB is less than half an hour. This is consistent with the observation that most patients recover consciousness rapidly within 2 hours.
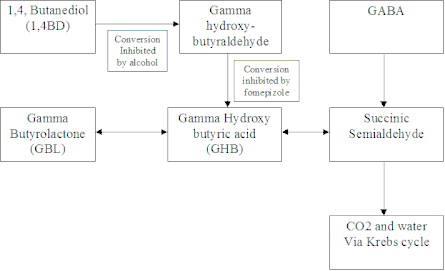
Substance and dosage:
Mostly liquid, though powder exists. Recreational dose varies greatly between solutions. Maximum dose per millilitre is 650mg. On average, recreational GHB consists of approximately 350mg/ml. Tubes usually contain 5ml.
GHB has medical uses in the treatment of narcolepsy and as anaesthetic.
The dose of GHB that is used to cause anaesthesia is 50mg/kg intravenously. The oral doses used in narcolepsy and for other indications are of the order of 25-100 mg/kg/day (typically about 500mg every 4 hours in adults).
Overdosage:
Possible overdose complications are seizures, bradycardia, respiratory arrest and coma.
A deep coma is characteristic of significant poisoning but generally short lived. The median time to recovery of consciousness is one hour. The most deeply sedated patients still generally recover fully within 6 hours. Endo-tracheal intubation and ventilation may be necessary, and deaths have occurred as a result of respiratory arrest. Patients may be briefly confused at the time of wakening.
Generalised tonic-clonic seizures, myoclonic jerks and absence seizures have all been reported but are not common. Status epilepticus does not occur and supportive treatment is probably all that is required for short-lived seizure activity.
Similar to other causes of coma, mild bradycardia, hypotension or hypothermia may occur. Hypotension responds rapidly to IV fluids. Dyskinesia, dystonia, vomiting and hallucinations may occur occasionally – perhaps due to secondary effects on dopaminergic function.
The majority of patients presenting to hospital have ingested other drugs – in particular alcohol and/or stimulants (e.g. amphetamines, MDMA, cocaine). This may lead to atypical presentations.
Both the release and inhibition pathways of GHB can be blocked by opioid antagonists such as naloxone and naltrexone, though no efficacy has been proven in clinical care.
Physostigmine has been proposed as an antidote for GHB, though there is little to no evidence of its clinical efficacy and serious adverse events have been described in its use.
Elimination enhancement is not indicated due to the very short half-life. Supportive care is usually all that is required. Patients should be nursed on their sides to help maintain their airway. Intubation and sometimes a short period of ventilation may be necessary.
Physostigmine for GHB coma http://www.tandfonline.com/doi/full/10.1080/15563650601072159
Treatment of narcolepsy with gamma-hydroxybutyrate. A review of clinical and sleep laboratory findings. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=3704454
Gamma-hydroxybutyrate serum levels and clinical syndrome after severe overdose https://linkinghub.elsevier.com/retrieve/pii/S0196064403003391
