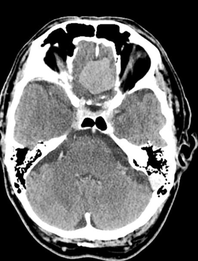
Meningioma
Meningiomas are dural based extra-axial tumors and represent the most common tumor of the meninges. Originating from the meningocytes or arachnoid cap cells of the meninges, they are located anywhere that meninges are found. Although they usually easily diagnosed, and are typically benign with a low rate of recurrence following surgery, there are a large number of histological variants with variable imaging features and, in some instances, more aggressive biological behaviour. Meningiomas typically have an iso-intense signal compared to grey matter on both T1 and T2 weighted imaging and enhance vividly on both MRI and CT.
Epidemiology
Meningiomas are more common in women, with a ratio of 2:1 intracranially and 4:1 in the spine. Atypical and malignant meningiomas are slightly more common in males. Meningeomas in patients under the age of 40 are rare and should raise suspicion of neurofibromatosis type 2 (NF2) when found in young patients.
Meningiomas are often easily recognised on CT imaging, though MRI may be used to confirm the diagnosis and extent of the lesion.
CT features
Non-contrast CT shows a slightly hyperdense image compared to normal brain in 60% of cases. The rest are more isodense. Up to 30% of lesions show calcifications. When contrast is given, 72% of meningiomas enhance brightly and homogeneously. Malignant or cystic variants may demonstrate more heterogeneity and less intense enhancement.
Hyperostosis is typical for meningiomas that abut the base of the skull. Enlargement of the paranasal sinuses (pneumosinus dilatans) has also been suggested to be associated with anterior cranial fossa meningiomas. Lytic and destructive regions are seen particularly in higher grade tumors, but should make one suspect alternative pathology (e.g. haemangiopericytoma or metastasis).